This is Part 2 of our series on short-chain fatty acids (SCFAs). In Part 1, we explored the fundamental role of SCFAs in maintaining a healthy gut microbiome. Now, we’ll examine the powerful effects of SCFAs beyond the gut, focusing on their significant impact on metabolic health. It turns out that these byproducts of gut fermentation play a crucial role in regulating blood sugar, influencing energy levels, managing appetite, and even promoting fat burning – highlighting the profound connection between gut health and overall metabolism.
What are Short-Chain Fatty Acids (SCFAs)? A Quick Recap
Short-chain fatty acids (SCFAs) are produced when beneficial bacteria in your colon ferment dietary fiber that resists digestion. The main SCFAs – acetate, propionate, and butyrate – are then absorbed and utilized by the body, influencing various physiological processes. For a detailed explanation of SCFA production and their role in gut health, see Part 1.
SCFAs and Metabolic Hormones: Influencing Appetite and Blood Sugar
SCFAs don’t just stay in the gut; they act as signaling molecules throughout the body. They enter the bloodstream and interact with various tissues, significantly influencing the release of key hormones that regulate appetite, blood sugar, and overall energy balance.
Appetite Regulation via Gut Hormones (GLP-1 & PYY)
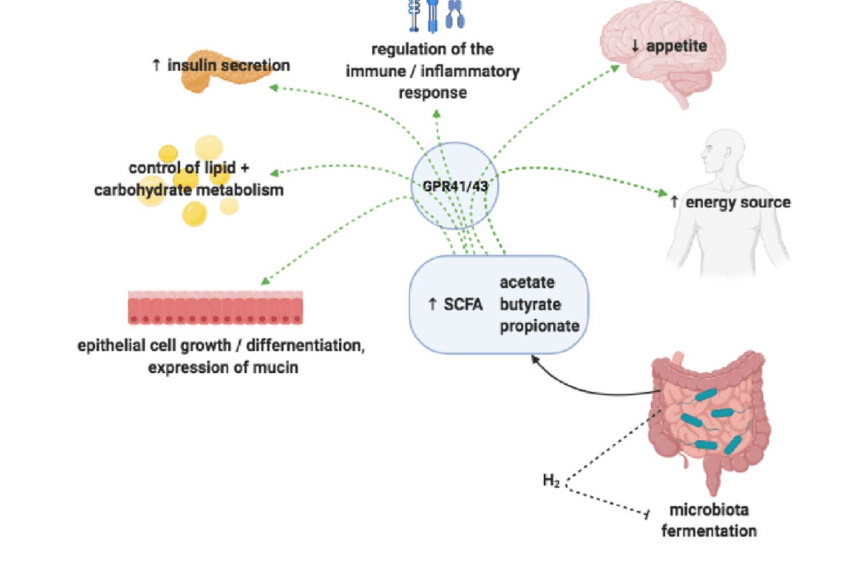
SCFAs, particularly butyrate and propionate, stimulate the release of glucagon-like peptide-1 (GLP-1) and peptide YY (PYY), hormones produced in the gut after eating. These hormones signal satiety (fullness) to the brain, helping to regulate food intake. GLP-1 specifically also increases insulin secretion, suppresses glucagon secretion (which raises blood sugar), and slows stomach emptying, further contributing to feelings of fullness. Studies, such as those involving inulin-propionate supplements, show that increasing colonic propionate production significantly boosts GLP-1 and PYY levels, potentially aiding weight management. You can read more about this in this study by Professor Gary Frost of Imperial College, London, Short chain fatty acids in the regulation of energy homeostasis.
Enhancing Glucose Metabolism and Insulin Sensitivity
SCFAs, especially propionate, play a crucial role in maintaining stable blood sugar levels. Propionate helps regulate glucose production in the liver. Furthermore, SCFAs can improve insulin sensitivity, meaning your body’s cells respond more effectively to insulin, allowing glucose to enter cells for energy. They interact with specific receptors known as free fatty acid receptors (FFARs, particularly GPR41 and GPR43) in various tissues, which influences both glucose and lipid metabolism, enhances insulin secretion, and improves glucose tolerance. This is vital, as impaired insulin sensitivity (insulin resistance) is a key factor in type 2 diabetes and other metabolic disorders. you can read more bout these clinical studies here.
SCFAs and Fat Metabolism: Influencing Fat Storage and Burning
Beyond hormone signaling, emerging research highlights the direct impact of SCFAs on how the body stores and utilizes fat. These gut metabolites interact with pathways that regulate energy expenditure and fat breakdown.
Promoting Fat Oxidation (Fat Burning)
SCFAs appear to encourage the body to burn fat more effectively. They activate essential pathways like AMPK, often called a “master switch” for metabolism, which promotes fat oxidation. They also influence PGC-1α, involved in mitochondrial biogenesis (creating more energy-producing units within cells), MDPI. This increased fat-burning capacity can contribute to better energy balance and potentially counteract the effects of high-fat diets.
Regulating Fat Storage
SCFAs may help regulate the amount of fat stored in adipose tissue (body fat). They activate receptors (like GPR41 and GPR43) found on fat cells, which can trigger signals to increase the breakdown of stored triglycerides and potentially inhibit the development of new fat cells. Research suggests SCFAs might offer protection against diet-induced obesity by enhancing energy expenditure and modulating fat storage pathways, MDPI.
This aligns with findings that SCFAs can act as a natural “obesity enzyme,” modulating hunger and metabolism through their effects on gut hormones.
These insights highlight the importance of dietary fibers and SCFAs in appetite regulation and weight management, suggesting that increasing SCFA-producing foods in the diet may be beneficial for controlling appetite and supporting metabolic health.
Supporting Lipid Metabolism and Cardiovascular Health
SCFAs, particularly acetate and propionate, also influence lipid metabolism more broadly. They can affect cholesterol synthesis and absorption, potentially contributing to healthier blood lipid profiles and reducing cardiovascular risk factors associated with metabolic dysfunction.
SCFAs and Inflammation: Impact on Metabolic Health
Chronic low-grade inflammation is increasingly recognized as a key driver of metabolic dysfunction, including insulin resistance and obesity. SCFAs possess potent anti-inflammatory properties that extend beyond the gut, helping to regulate systemic inflammation and support metabolic health.
Modulating Inflammatory Cytokines
To understand how SCFAs combat inflammation linked to metabolic issues, we need to look at cytokines. Think of cytokines as tiny protein messengers used by your immune system to communicate. Some cytokines act like alarm bells, promoting inflammation to fight infection or injury, while others act to calm things down. Maintaining a healthy balance is key.
Two major players often involved when inflammation becomes problematic are:
- TNF-α (Tumor Necrosis Factor-alpha): This is a primary pro-inflammatory cytokine. It’s often one of the first responders released during an inflammatory event, signaling other immune cells to join the fight. While essential in moderation, chronically elevated TNF-α is linked to various inflammatory conditions, including insulin resistance.
- IL-6 (Interleukin-6): This is another crucial cytokine, often released following TNF-α signals. IL-6 has complex roles – it can be pro-inflammatory, especially in chronic conditions like obesity and type 2 diabetes, contributing to systemic inflammation. However, it also has some anti-inflammatory roles in other contexts. An imbalance, particularly chronic elevation, is linked to metabolic dysfunction.
Research shows that SCFAs, particularly butyrate, can help restore balance by modulating these powerful signals. They can suppress the production and activity of pro-inflammatory cytokines like TNF-α and IL-6, while potentially boosting anti-inflammatory pathways. They achieve this by influencing specific signaling pathways within immune cells and other cell types, helping to prevent the chronic, low-grade inflammation that undermines metabolic health. You can more more about in publication, The role of SFCA in Innflammation and overall Health.
Supporting Immune Balance (Regulatory T Cells)
SCFAs are crucial for the development and function of regulatory T cells (Tregs). These specialized immune cells help maintain immune balance, preventing excessive inflammatory responses and autoimmune reactions. By promoting Treg function, SCFAs contribute to a less inflammatory internal environment, which is beneficial for metabolic health.
Impact on Muscle Inflammation
An imbalance or deficiency in SCFAs may contribute to increased inflammation in muscle tissue. As SCFAs modulate immune responses, adequate levels may help reduce muscle inflammation associated with conditions like sarcopenia (age-related muscle loss) and support muscle repair and function.
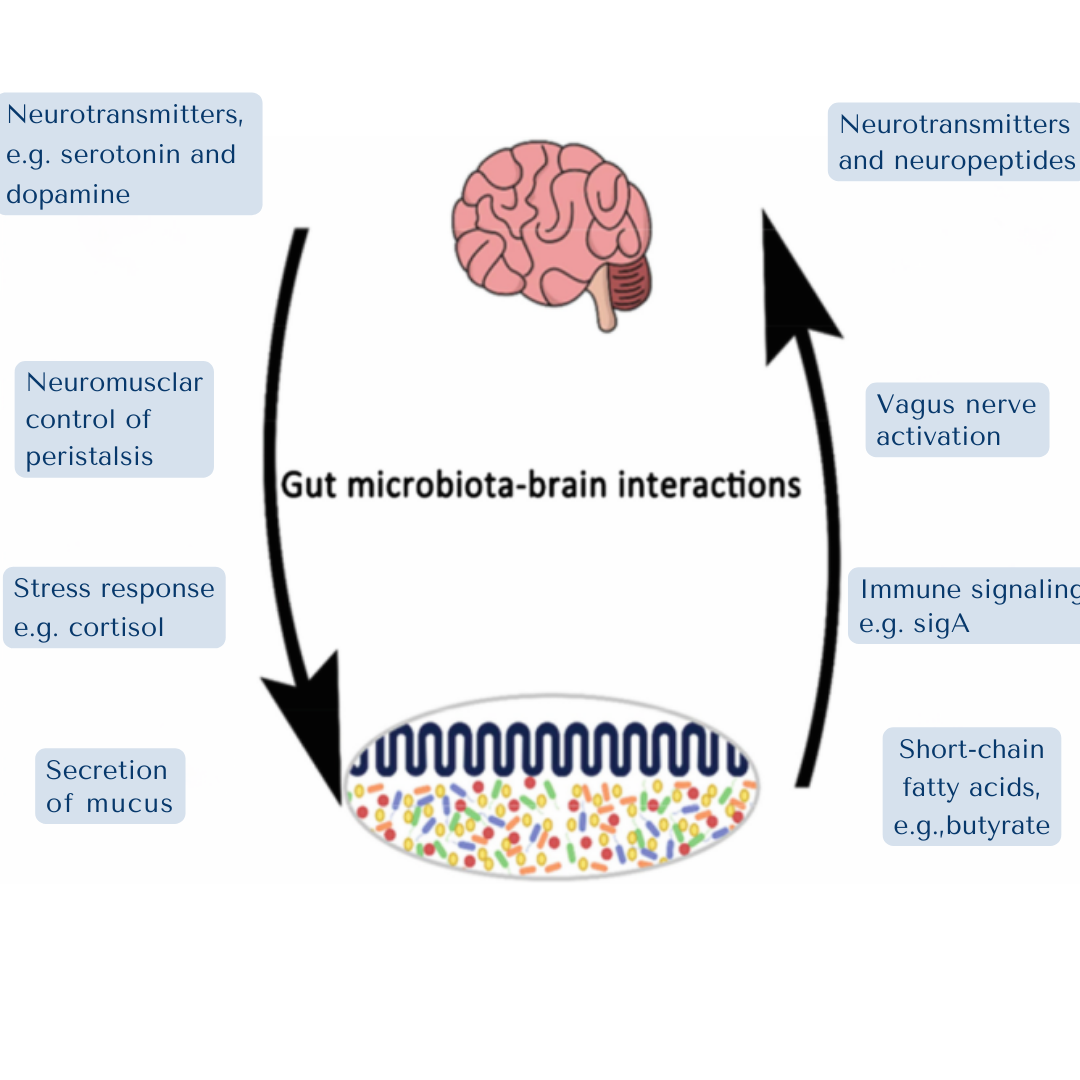
The Gut-Brain Axis: SCFAs Influence Stress, and Cognition
The gut and brain are intricately connected through the gut-brain axis, a complex communication network. SCFAs produced in the gut play a vital role in this communication, influencing neurotransmitter production, stress responses, mood, and cognitive function – all of which can indirectly impact metabolic health.
SCFAs and Neurotransmitter Production
Remarkably, gut bacteria and SCFAs influence the production of key neurotransmitters. For instance, butyrate has been shown to play a role in serotonin synthesis within the gut; approximately 90% of the body’s serotonin (“feel-good” neurotransmitter) is produced there. Balanced SCFA levels thus support stable mood and emotional well-being.
Impact of Mental Health & Stress on SCFAs
The gut-brain connection is bidirectional. Chronic stress, anxiety, and depression can negatively impact gut microbial diversity, reducing the abundance of SCFA-producing bacteria like Faecalibacterium prausnitzii (a key butyrate producer). This reduction in SCFAs can worsen gut barrier dysfunction (“leaky gut,” discussed in Part 1) and inflammation, potentially creating a vicious cycle that impacts both mental and metabolic health. You can learn more about the Gut- Brain axis in our dedicated article.
Modulating Emotion and Cognition
Beyond mood, SCFAs entering the bloodstream can cross the blood-brain barrier or signal via pathways like the vagus nerve to influence brain function, potentially modulating emotion and cognitive processes. Research in this area is rapidly evolving.
SCFAs, Autophagy, and Cellular Health
The metabolic influence of SCFAs extends to fundamental cellular processes like autophagy. Autophagy (meaning “self-eating”), derived from the Greek words for “self” (auto) and “eating” (phagy), is the body’s natural recycling system, removing damaged components and maintaining cellular health, which is crucial for healthy aging and preventing metabolic dysfunction.
SCFAs and Autophagy Stimulation
Research indicates that SCFAs, particularly butyrate, can stimulate autophagy pathways, PubMed. By promoting this cellular cleanup process, SCFAs help maintain cellular efficiency and resilience, which is vital for preventing the accumulation of damage that contributes to age-related metabolic decline and disease. Enhancing autophagy is increasingly recognized as a key factor in promoting longevity and healthy aging. You can read more about Butyrate production and heath benfits in our dedicated article, What is Butyrate Role for Gut and Overall Health.
The Gut-Metabolism Link to Energy Levels
The profound connection between your gut health, SCFA production, and daily energy is clear. A well-functioning metabolism, influenced positively by SCFAs and supported by reduced systemic inflammation and a balanced gut-brain axis, is essential for sustained vitality.

Fueling the Body Efficiently
Fueling the Body Efficiently By contributing to stable blood sugar, efficient fat burning, healthy cellular function (via autophagy), reduced inflammation, and potentially a more balanced mood/stress response, SCFAs help ensure your body produces and utilizes energy effectively. Boosting SCFA production through diet is key – see Part 1 for detailed dietary strategies.
Conclusion
Fueling the Body Efficiently By contributing to stable blood sugar, efficient fat burning, healthy cellular function (via autophagy), reduced inflammation, and potentially a more balanced mood/stress response, SCFAs help ensure your body produces and utilizes energy effectively. Boosting SCFA production through diet is key – see Part 1 for detailed dietary strategies
Guan, L. L., de Bruijn, W. J., Choong, Y. S., & Solis, G. (2019). Fermented Rice Bran and Rice Bran Oil in Traditional Japanese Medicine: Sake as a Potential Functional Beverage. Journal of Ethnopharmacology, 235, 405-418. https://doi.org/10.1016/j.jep.2019.01.007
Lee, D. E., Huh, C. S., & Huh, J. W. (2019). Korean Traditional Use of Fermented Rice Water: A Historical Review and its Modern Applications in Cosmetics. Journal of Cosmetic Science, 70(3), 241-250.
Zhou, J., & Qu, F. (2015). Face Mapping: Chinese Holistic Skin Analysis as an Indicator of Internal Organ Imbalance. International Journal of Dermatology, 54(8), 884-892. https://doi.org/10.1111/ijd.12736
Bowe, W. P., & Logan, A. C. (2011). Acne vulgaris, probiotics and the gut-brain-skin axis – Back to the future? Gut Pathogens, 3(1), 1. https://doi.org/10.1186/1757-4749-3-1
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC10385652
https://www.mdpi.com/1422-0067/24/24/17618
https://journals.plos.org/plosone/article?id=10.1371/journal.pone.0237207
Join Us in Redefining Beauty
Subscribe for Exclusive Insights









